Recurrent Primary Mucinous Eccrine Adenocarcinoma Sensitive to Radiation Therapy
Ben Goodman, OMS III
Pikeville College School of Osteopathic Medicine
6610 Valley Forge Court
Indianapolis, IN 46237
Bill Giese, MD JD
Progressive Radiation Oncology
Regional Cancer Center
Murray-Calloway County Hospital
204 South 9th St., Suite B
Murray, KY 42701-2409
INTRODUCTION
Mucinous eccrine adenocarcinoma (MEA) is a malignant neoplasm of eccrine origin. It is usually seen in the head and neck region, with a tendency to originate from the eyelid and periorbital region. [1, 2]This tumor is very rare, with less than 130 cases described in the literature to date. [3] Due to its rarity and similar histologic features to mucinous adenocarcinomas of noncutaneous origin, a true diagnosis cannot be made until metastasis from other primary organs has been ruled out. Primary tumors that may metastasize to the skin and produce mucin are breast, gastrointestinal tract, lung, kidney, ovaries, pancreas, and prostate. [1, 3] Primary MEA occur more often in men than women with a 2:1 ratio. This occurs most commonly at a mean age of sixty-three years, but there have been reports of rare cases in children. [2, 4] Local recurrence is very commonly seen. We report a case of recurrent primary MEA in an elderly man that had recurred with previous surgical procedures, but proved to be sensitive to radiation therapy.
CASE DESCRIPTION
An 89-year-old caucasian male presented to our practice with an eight year history of primary MEA involving the skin of the left medial canthus. The patient wanted to review the possible treatment options for a rare and clinically recurrent eccrine sweat gland neoplasm.
Eight years prior to presentation, the patient had a raised, soft lesion surgically removed from the medial canthal area of his left eye. The tumor was locally excised a second time one year later due to clinical evidence of recurrence. The specimen was sent to pathology after the rapid recurrence. The pathology report identified the mass as a mucinous eccrine adenocarcinoma.
Three years later, the patient noticed a third recurrence of the tumor, but did not seek medical attention at that time. The patient admitted that the tumor mass had been increasing in size, and it was beginning to interfere with his left eye�s medial field of vision.
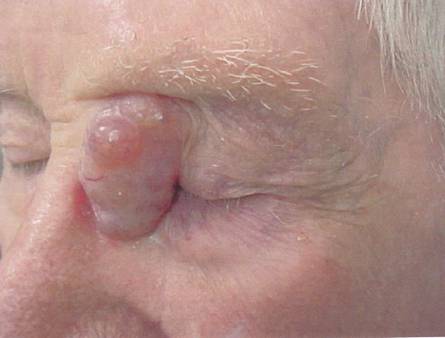
A raised, freely mobile, and soft skin mass of approximately 4.0 x 4.0 cm, and raised 3.0 cm, was present on the medial canthal region on the left eye (Figure 1). The patient�s extraocular eye movements were unaffected. Examination revealed no other suspicious skin lesions or palpable lymph nodes present.
A whole body PET/CT scan confirmed a soft tissue density in the left upper canthal region of equivocal hypermetabolic activity. This was also done to rule out possible metastasis from any other primary site. A full baseline vision evaluation was performed by his ophthalmologist. Unfortunately, he refused the dilation needed to get a good look at his eye grounds and complete the evaluation. A whole body skin check by his dermatologist identified no other suspicious lesions.
The patient was informed in great detail regarding the management of this unusual type of cancer in general, and the specifics of his particular case. He presented refusing re-biopsy but with clinical evidence of tumor recurrence. Our practice, along with his other managing physicians, presented the patient with the surgical treatment options. He remained adamant, that he would not consent with a plastics reconstructive expert due to recurrence with previous surgeries.
The patient was counseled suggesting benefit from systemic tamoxifen alone. This appeared to be limited to those patients who are estrogen receptor (ER) positive. Due to the patient�s refusal to re-biopsy the present lesion, the pathologist was able to conduct ER immunohistochemical stains on the previous specimens that were removed eight years prior. Indeed, the tissues biopsied previously were ER positive.
Local irradiation was known to be with some risk and we discussed in detail the potential treatment-related complications. The risk would be reduced by employing en face electrons, and sufficient overlying lead shielding placed daily during treatment. High-energy electrons would provide full tumor dosing based on the tumor extent as defined on physical examination and what was seen on the PET/CT. Electrons also provide for rapid reduction of dose deep. This would prevent significant exposure to his retina, and optic nerve.
Tamoxifen 10mg by mouth twice a day was initiated accordingly, due to the tumor proving positive for estrogen receptors. The patient was asked to carefully consider his options, including a trial of tamoxifen alone or adjuvant treatment with radiation therapy. He opted for tamoxifen with simultaneous irradiation. The patient discontinued the tamoxifen two weeks later against medical advice because he felt that it was of no benefit.
The initial dose of irradiation was given in the left inner canthus site. The field size was 5 x 5 cm via a 3 x 3 cm electron cut-out. The mode of energy was 14 MeV electrons. 200 cGy was given daily via a single en face electron portal. Treatments were conducted five days per week. This was a total dose of 7,000 cGy in 35 fractions over 51 elapsed days.
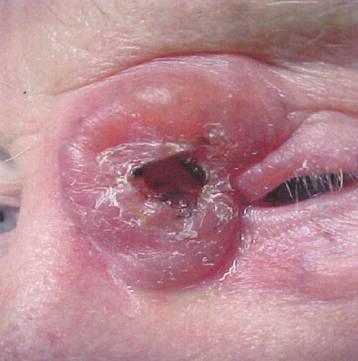
At the conclusion of the initial treatment, minimal tumor response was seen, but the patient tolerated the course of local irradiation well. He did, however, develop some local skin erythema, and desquamation, as expected (Figure 2).
While he was followed closely during the months following his initial course of irradiation, where 7,000 cGy was delivered, there was some involution of this left-sided medial mass centrally. Over the ensuing few months, though, the tumor mass failed to show further response. The patient continued to categorically refuse to consider any attempt at surgical re-excision of the lesion. We discussed with the patient the possible delivery of additional local irradiation. Due to the disease location, in particular the proximity to the left inner eye, the second dose of en face electrons was limited, but unlikely to cause further injury to the deeply located optic nerve or chiasm.
The patient requested to proceed with a second dose of irradiation. The second dose of irradiation was also given in the left inner canthus site. The field size was 5 x 5 cm cone via a 3 x 3 cm electron cut out. The mode of energy was 14 MeV electrons via an en face yet custom cut-out port. 200 cGy was given daily via a single en face electron portal. Treatments were conducted five days per week. This was a total dose of 3,000 cGy in 15 fractions over 21 elapsed days.
The patient tolerated the second course of localized irradiation well. He did again develop minor skin erythema within the treated region, but no frank tissue breakdown. He remained without vision changes or conjunctival inflammation by course completion.
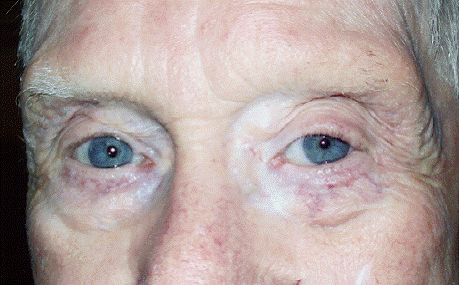
There continued to be clinical response to the irradiation. Over time the patient�s tumor continued to respond centrally and peripherally. Now more than three years after the initial irradiation treatment, the patient continues to improve (Figure 3).
DISCUSSION
Primary MEA is a very rare, slow growing malignant tumor with less than 130 known cases to date. The tumor�s greatest occurrence is seen in the eyelid and periorbital region. [1,2] Primary MEA occurs more often in men than women with a 2:1 ratio. This occurs most commonly with a mean age of 63 years, but there have been reports of rare cases in children. [2,4] More than two-thirds of those affected are white. [5] MEA is painless and is usually ignored by the patient for a substantial period of time. There is a very high propensity for local recurrence as evidenced by this case, but metastases are rare. [6,7] Mucinous adenocarcinomas can also present in the breast, gastrointestinal tract, lung, kidney, ovaries, pancreas, and prostate. [3] Clinically, the appearance can present variably as bumpy, smooth, firm, crusted, papillomatous, pedunculated, and fungating. The color can also vary with a wide range of yellow, tan, blue, pink, reddish brown, and red. Histologically, it is hard to differentiate primary MEA from metastatic MEA. Primary lesions can be differentiated from metastatic lesions by their more organized epithelial cells, less hyperchromasia and fewer mitoses in individual cells. Due to the difficulty in distinguishing these histologically, a thorough work-up for metastatic lesions should be completed with any new diagnosis. [4] The patient in this case report had a complete PET/CT which was insignificant for any other primary location.
Previous literature has suggested Mohs micrographic surgery as the mainstay of treatment. Our case report demonstrates that with the recent advancements in the field of radiation oncology, radiation therapy could possibly become the treatment of choice. There have been only three other reports of successful post-surgical adjuvant radiotherapy that showed no signs of recurrence 18-48 months after treatment. [2] En face electrons are not deeply penetrating and do not post a large risk of possible side effects. Other than some slight eczema and erythema, no other side effects were noted with this patient.
REFERENCES
Kelly BC, Koay J, Driscoll MS, Raimer SS, Colome-Grimmer MI. Report of a case: Primary mucinous carcinoma of the skin. Dermatol Online J. 2008; 14(6):4.
Durairaj VD, Hink EM, Kahook MY, Hawes MJ, Paniker PU, Esmaeli B. Mucinous eccrine adenocarcinoma of the periocular region. Opthal Plast Reconstr Surg. 2006; 22(1):30-5.
Bindra M, Keegan DJ, Guenther T, Lee V. Primary cutaneous mucinous carcinoma of the eyelid in a young male. Orbit. 2005; 24(3):211-4.
Cabell CE, Helm KF, Sakol PJ, Billingsley EM. Primary mucinous carcinoma in a 54-year-old man. J Am Acad Dermatol. 2003; 49(5):941-3.
Gupta A, Flowers FP, Lessner AM. Asymptomatic eyelid papule in a 57-year-old healthy man. Arch Dermatol. 2000; 136(11):1409-14.
Sudesh R, Siddique S, Pace L. Primary eyelid mucinous adenocarcinoma of eccrine origin. Ophthalmic Surg Lasers. 1999; 30(5):394-5.
Boynton JR, Markowitch W Jr. Mucinous eccrine carcinoma of the eyelid. Arch Opthalmol. 1998; 116(8):1130-1.